Treating Joint Pain in a Natural Way
- Details
- Written by: Joanne Wallenstein
- Category: Health
 Contributed by Dr. Nicole Solomos, Lifestyle Medicine. The original version of this article was published in Health Matters, a White Plains Hospital publication.
Contributed by Dr. Nicole Solomos, Lifestyle Medicine. The original version of this article was published in Health Matters, a White Plains Hospital publication.
Nagging joint pain can affect not just your body, but also your mind and your mood. As a result, many people suffering from joint pain do so by remaining relatively sedentary, afraid that engaging in physical activity will only exacerbate their situation.
However, as a practitioner of lifestyle medicine, I strongly recommend that everyone – and not just those with joint pain – follow certain regimens that can help them change their lives for the better. Lifestyle medicine is a medical specialty that uses therapeutic lifestyle interventions as a primary technique in treating chronic conditions.
For the purposes of this article, I will be speaking in generalities; obviously, each individual is facing their own situation, and some are more capable of making these adjustments than others. Nevertheless, following these recommendations can help those with joint pain feel refreshed, renewed, and more able to deal with their challenges.
Regular physical activity/exercise. This cannot be stressed enough. Such activity can keep the muscles around affected joints strong, slow the loss of lean mass, and in some cases can help control joint swelling and pain. In addition, regular activity can help restore lubrication to the cartilage of the joint, thereby reducing stiffness and pain.
This proposal may strike some – especially the elderly and/or those with severe joint pain – as difficult to achieve. But that is not necessarily the case. Strength training, which has not been emphasized enough in our culture, can be done at any age (it’s never too late to start!) and doesn’t necessarily mean lifting large barbells or dumbbells over your head repeatedly. Body weight exercises like push-ups or modified squats can be a great way to start; there is a host of exercises utilizing chairs for extra support. Resistance training, done with resistance bands, sandbags, or even some household items are also recommended, as are core exercises like planking or others that involve lying on your back.
Remember: strength and mobility can be more important than emphasizing one’s weight or body size; they can even go hand in hand. You aren’t looking to compete in the next Iron Man; you are looking to get more fit and relieve the stress on your aching joints.
Nutrition. Defining what makes for a “proper” nutrition plan can be complicated; there is no one way that’s right for everyone. For that reason, I recommend that each person comes up with their own customized eating plan rather than relying solely on someone else’s suggestions. The latter will usually prove to be unsustainable, and you might simply give up after a few weeks or months.
That said, I consider the Mediterranean diet to be the gold standard, with its emphasis on plant-based foods and healthy fats; details can be found here. Processed foods should be avoided, and you should be aware that your preferred intake of protein will vary as you get older, especially for women; those in peri- or post-menopause should be eating differently than those who are pre-menopause.
Risky substances. We all know (or should know) that smoking is a habit that should not be indulged. The same is true for alcohol; despite its normalization in our society – how many beer commercials do you see during a televised sporting event? – I feel that alcohol should be cut out of one’s life entirely. I realize that isn’t a particularly popular notion, but if you can’t keep it down to 0 drinks a week, try to limit it to no more than two drinks a day for men and no more than one drink a day for women, as the CDC suggests.
Caffeine is also a risky substance. Again, moderation is key; I feel that a single cup in the morning should be sufficient. Otherwise, you may be prone to feeling jittery/nervous, dehydrated, and/or having an increased heart rate. Too much caffeine or alcohol can have a negative impact on your sleep – and, thus, on your joint pain.
Sleep. An adequate amount of sleep allows your body to maintain healthy brain function and good physical health. Joint pain can result in restless sleep – without movement, your joints can stiffen during the night – and a lack of sleep can aggravate the pain. The exercises and other healthy habits listed above can help alleviate this problem.
Less than the recommended 7 to 8 hours a night may increase your chances of not only exacerbating joint pain, but also in developing chronic health problems. Dr. Nicole SolomosWater. Drinking enough water each day is one of the keys to sustaining a healthy lifestyle. The general guideline here is to take in at least 64 ounces of water a day (age, sex and activity levels may alter that recommendation). Water helps in maintaining healthy tissue as well as healthy joints. Water also is an excellent alternative to alcohol for a number of reasons; in addition, it can help fill you up, thus eliminating the urge for between-meal snacks.
Dr. Nicole SolomosWater. Drinking enough water each day is one of the keys to sustaining a healthy lifestyle. The general guideline here is to take in at least 64 ounces of water a day (age, sex and activity levels may alter that recommendation). Water helps in maintaining healthy tissue as well as healthy joints. Water also is an excellent alternative to alcohol for a number of reasons; in addition, it can help fill you up, thus eliminating the urge for between-meal snacks.
Following these guidelines will probably not eliminate your joint pain, especially if you have a chronic condition like arthritis. But it can definitely help alleviate at least some of it, which in turn will result in feeling both happier and healthier.
Dr. Nicole Solomos is board-certified in Sports Medicine/Family Medicine and in Lifestyle Medicine. To make an appointment, call 914-849-7075 (Somers) or 914-631-7777 (Hawthorne and Yonkers).
Tips for Men’s Health
- Details
- Written by: Joanne Wallenstein
- Category: Health
 This article was written by Dr. Matthew Zeppieri, Family Medicine
This article was written by Dr. Matthew Zeppieri, Family Medicine
Remembering to prioritize your physical and mental health can be challenging, especially while balancing work, social life, and family. Despite this, it is important for men to follow some basics in order to remain healthy and prevent future illness.
1. Attend Annual Physicals
Given the high likelihood of prostate and colon cancer in men, it is important to schedule annual physicals. In addition to prostate cancer, colorectal cancer is more common in men. While men and women are essentially equally at risk for colon cancer, men are more likely to get rectal cancer, according to the Centers for Disease Control and Prevention (CDC). Both prostate and colorectal cancer screenings can be critically important, as the earlier those diseases are detected, the better the chances of successfully treating them.
With patients under 40, I inquire if they are experiencing any typical prostate cancer symptoms, including multiple trips to the bathroom at night to urinate; general frequency and urgency associated with urinating; and hesitancy or weakening of the urine stream. Other concerning indications include unexplained fevers and/or unintentional weight loss.
With patients over 40, I recommend conducting a Prostate Specific Antigen (PSA) screening and a digital rectal exam. Although some patients are more resistant to these procedures that others, there is value in conducting these screenings and catching these illnesses early on.
With colon cancer, since we are finding an increase in cases of younger men, the recommended age for a colonoscopy has been lowered from 50 to 45. In addition, if an individual has a family history of colon cancer, it is recommended that a screening be done 10 years prior to when that family member’s diagnosis took place.
2. Active Lifestyle
The American Heart Association recommends 150 minutes of moderate exercise weekly. This type of exercise includes any activity other than sitting at a desk – including, but not limited to, household chores or going for short walks.
Another option to maintain an active lifestyle is 75 minutes of vigorous exercise weekly. This type of exercise includes a more intense regimen like jogging, swimming, playing racquetball, etc. With both of these options, the overarching goal is to remain active regardless of the ways in which that activity is accomplished.
3. Balanced Diet
Maintaining a balanced diet and consuming the appropriate amount of calories can be difficult, given the multitude of different diet options and discussions around calorie intake. Daily calorie intake recommendations are 2,400 for those aged 21 to 40; 2,200 for those aged 41 to 60; and 2,000 for men aged 61 and older. To lose one pound a week, those numbers can be decreased by 500 calories.
I recommend accurately counting your calorie intake. It is important to be honest with your physician and yourself when calorie counting, as inaccurate reporting does not help your physician – or, more importantly, yourself.
A diet that I and many other physicians recommend is the Mediterranean diet, which emphasizes plant-based foods and healthy fats. Additional details can be found here. 4. Monitor Mental Health
4. Monitor Mental Health
Checking up on the mental health of my patients is a priority. Every time I see a patient, I always inquire about feelings of depression, anxiety and stressors in their lives. Given the still-present stigma around their emotional needs, it can be hard for some men to openly discuss their mental health with their physician. Despite this, it is imperative to have these discussions with your physician, instead of allowing an illness to remain untreated.
Again, it is vital to prioritize receiving your annual physical and age-appropriate screenings as a preventative measure to remain safe and healthy. If you have not already done so, I urge you to schedule any visits that you may have let slip by; your doctor, and your body and mind, will thank you.
Dr. Matthew Zeppieri is a family medicine physician at White Plains Hospital Physician Associates of New Rochelle. For an appointment, call 914-235-8224.
Living with Lupus: Symptoms, Diagnosis, and Effective Treatment Strategies
- Details
- Written by: Dr. Petros Efthimiou, Rheumatology
- Category: Health
 Systemic Lupus Erythematosus (SLE), a.k.a “lupus,” has been back in the news lately, with actress/singer Selena Gomez and vocalist Toni Braxton making headlines for their experiences with the autoimmune disease. Earlier this year, Gomez began openly discussing the effects of lupus, which she was diagnosed with in 2015; more recently, Braxton, who was diagnosed in 2008, has publicly shared her experience with lupus and one of its major complications, lupus nephritis, where the disease affects the kidney.
Systemic Lupus Erythematosus (SLE), a.k.a “lupus,” has been back in the news lately, with actress/singer Selena Gomez and vocalist Toni Braxton making headlines for their experiences with the autoimmune disease. Earlier this year, Gomez began openly discussing the effects of lupus, which she was diagnosed with in 2015; more recently, Braxton, who was diagnosed in 2008, has publicly shared her experience with lupus and one of its major complications, lupus nephritis, where the disease affects the kidney.
The Mayo Clinic defines lupus as Lupus can be defined as Lupus is “a disease that occurs when your body’s immune system attacks your own tissues and organs (autoimmune disease). Inflammation caused by lupus can affect many different body systems – including your joints, skin, kidneys, blood cells, brain, heart and lungs.”
With May being Lupus Awareness Month in the U.S., it is worth discussing the potential symptoms of, as well as treatments for, this disease whose name might be familiar but whose details may be murky for many readers. 
The Lupus Foundation of America (LFA) reports that about 1.5 million Americans have the disease, with an estimated 16,000 new cases diagnosed each year. Worldwide, over five million people have some form of lupus. While it is most common in women between the ages of 18 and 45, it can also affect men; in addition, the disease currently affects an estimated 5,000 to 10,000 children.
Lupus can affect almost any organ in the human body; not just the kidney, but also the skin, blood, joints, heart, lungs, and brain. Fatalities directly attributable to the disease are few; with close follow-up and treatment, 80-90% of people with lupus can expect to live a normal life span, according to the LFA.
There is no cure for lupus, and the exact cause(s) of contracting it are yet to be conclusively identified. However, there appears to be a genetic factor at play; while no single gene or gene group has been proven to cause the disease, it can appear in some families. People of African, Asian, Pacific Island, Hispanic/Latino, Native American or Native Hawaiian descent are more susceptible to lupus, again indicating a possible genetic factor.
Common triggers of the disease include infection or injury; overwork/lack of sleep; and prolonged exposure to the sun or fluorescent/halogen light. Symptoms may include:
• Muscle and joint pain
• Prolonged fever
• Rashes
• Chest pain
• Hair loss
• Sun or light sensitivity
• Kidney issues
• Mouth sores
With all of this uncertainty, how can one tell if they do have lupus? The prolonged presence of these symptoms – especially if one more than one is present at a time – should be taken seriously. A visit to your physician should quickly be arranged; blood and urine tests can screen for the disease, and you may ultimately need to be referred to a rheumatologist, who can confirm the diagnosis and prescribe a treatment, tailored to your clinical presentation.
If you are found to have lupus, there are many treatments available. Depending on the person and the severity of the case, these range from antimalarials, such as hydroxychloroquine, to the corticosteroid prednisone, all of which can help reduce swelling, tenderness and pain. Immunomodulators such as azathioprine and mycophenolate can also prove effective, and for severe cases, targeted biologic immunotherapy may be recommended.  Dr. Petros Efthimiou In any event, close supervision by a rheumatologist is highly advised. They can help find the right approach to the disease for you and guide you on what may be a difficult – but not necessarily life-threatening – journey.
Dr. Petros Efthimiou In any event, close supervision by a rheumatologist is highly advised. They can help find the right approach to the disease for you and guide you on what may be a difficult – but not necessarily life-threatening – journey.
Dr. Petros Efthimiou is a board-certified rheumatologist and a published lupus expert at WPHPA of Larchmont. For an appointment, call 914-849-7400.
Relief Without the Sting: How Allergy Pills Are Changing the Game for Treatment
- Details
- Written by: Dr. Angela Chan
- Category: Health

Seasonal allergies can be irritating not just for the upper airways, but also for the eyes. Seasonal allergic rhinitis (hay fever) is an allergic response to airborne pollens such as trees, grasses, and weeds, which can be particularly bothersome as it spans from early March to the first frost, here in the tri-state area.
According to the Asthma and Allergy Foundation of America, in 2021 some 81 million people in the U.S. were diagnosed with seasonal allergic rhinitis – equal to about 26% (67 million) of adults and 19% (14 million) of children.
The “seasonal” part of the equation can be defined by these simple facts: Tree pollen is common in spring; grass pollen in late spring into summer; and ragweed pollen in late summer into fall. And as unpleasant as dust mites and cockroaches sound, these allergens, along with animal dander, are present year-round, and are considered triggers for perennial symptoms.
Once diagnosed, allergic rhinitis treatment options include avoidance (if possible) and eliminating or decreasing your exposure to the triggers. This can of course be difficult to achieve in the case of pollen unless one lives roughly three quarters of the year indoors. Alternatively, with regards to dust mites, no matter how clean your home is, it is probably still a little dusty.
Treatments that patients initially rely on for their allergies include antihistamines (oral, intranasal, ocular), and intranasal corticosteroids, which provide temporary symptomatic relief. Allergen immunotherapy (also known as allergy shots) has been shown to be effective in treating patients with allergic rhinitis. Unlike allergy medications, allergy shots modify the underlying cause of the disease and can provide long-term benefits. However, patients can find it challenging to commit to the recommended allergy regimen: weekly injections for about six months to build their tolerance to the allergen(s), followed by a maintenance schedule of once monthly injections for the next three to five years.
Fortunately, there is another type of treatment available: sublingual immunotherapy (SLIT). This involves allergy tablets and has emerged as an effective, safe, and possibly more feasible alternative to allergy shots for some individuals. Currently in the U.S., the FDA has approved four allergy tablets: two are directed at grass pollen (Oralair and Grastek); one is for short ragweed (Ragwitek); and one is for dust mites (Odactra). Oralair, Grastek, and Ragwitek are approved for children 5 years old and above. Odactra is approved for children 12 years old and above.
The tablets are placed under the tongue for at least one minute, then swallowed as they dissolve. They are generally taken once a day during therapy. The dosing regimen varies depending on the targeted allergen, where one could benefit from starting SLIT several months before the season (as with pollens), while others may benefit from year-long SLIT (as with dust mites). Treatment typically is continued for around three years for continued effectiveness.
Side effects of allergy tablets are usually mild for all ages: itchy mouth (if present, would occur early in treatment and usually is transient) and, less commonly, an upset stomach. Severe allergic reactions are rare; however, as there is the possibility of severe allergic reactions in patients receiving immunotherapy (whether allergy tablets or allergy shots), for safety purposes, an epinephrine autoinjector is always prescribed.
SLIT is only appropriate to consider for certain patients who have allergic rhinitis to the allergen contained in the allergy tablet of choice. As such, patients with multiple allergies would likely benefit from allergy shots instead.
Knowing that they may be able to “breathe easier” without injections is an attractive option for many patients; however, whether these tablets are adequate or recommended for you is a matter for discussion with an allergist.

Dr. Angela Chan is a board-certified pediatrician and allergist-immunologist at the Scarsdale Medical Group in Harrison. For an appointment, please call 914-723-8100.
150 Scarsdale Residents Learn CPR
- Details
- Category: Health
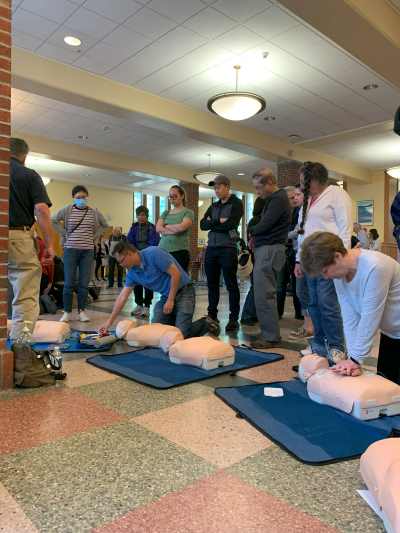
 According to the National Heart, Lung, and Blood Institute, cardiac arrest results in about 300,000 to 450,000 deaths in the United States each year. Cardiac arrest is a medical emergency that requires immediate medical attention—90% of people who have a cardiac arrest outside of a hospital die within minutes due to insufficient blood flow to vital organs. However, the American Heart Association states that the immediate administration of cardiopulmonary resuscitation (CPR) to a patient can double or even triple that person’s chance of survival.
According to the National Heart, Lung, and Blood Institute, cardiac arrest results in about 300,000 to 450,000 deaths in the United States each year. Cardiac arrest is a medical emergency that requires immediate medical attention—90% of people who have a cardiac arrest outside of a hospital die within minutes due to insufficient blood flow to vital organs. However, the American Heart Association states that the immediate administration of cardiopulmonary resuscitation (CPR) to a patient can double or even triple that person’s chance of survival.
Recognizing that bystander intervention is a critical aspect of pre-hospital care, Scarsdale Volunteer Ambulance Corps (SVAC) organized a Friends & Family CPR Class at the Scarsdale Public Highschool. Morning and afternoon training sessions were hosted on May 7th, 2023, where a total of 150 residents learned how to perform hands-only CPR. The program was truly a community effort, with instructors from SVAC, Larchmont Volunteer Ambulance Corps, and Irvington Volunteer Ambulance Crops attending to teach. The combined effort of the participating organizations was essential to the success of the program.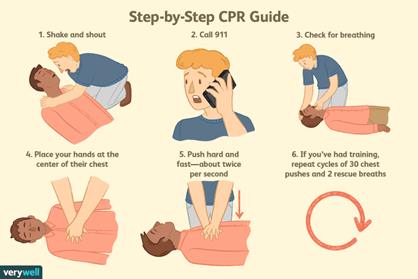
According to Angela Manson, a dedicated member of SVAC, the organization is always looking for new volunteers. Manson stated that SVAC runs year-round EMT classes and that no experience is needed to participate in their programs. Above all, she emphasized that the programs would equip participants with the knowledge and skills needed to manage medical emergencies. More information on available courses can be found here.