Should You Invest in a Weighted Vest?
- Details
- Written by: Joanne Wallenstein
- Category: Health
 (Submitted by Dr. Mark Klion, Orthopedic Surgery at White Plains Hospital)
(Submitted by Dr. Mark Klion, Orthopedic Surgery at White Plains Hospital)
The latest workout trend is wearing a weighted vest. Once a tool for soldiers and policemen, weighted vests today seem to be everywhere – you may see them in use at the gym, on a leisurely walk, or even at your workplace. It seems that everybody from your friend to your postman and even your physician (yes, that includes me) is trying one on for size.
But is the weighted vest something destined to go the way of high-fat diets, the ThighMaster, and the Jazzercise class – or is it something with a high longevity potential? In this article, I will review its history, how it works, and the pros and cons of wearing one.
Ten-Hut!
The weighted vest actually dates back to such civilizations as the ancient Greeks, who filled leather vests with sand or stones to help train their soldiers for combat. Likewise, vests are used by many of today’s military and police units to simulate the extra weight of body armor and equipment during training exercises.
The term “rucking” also originates with the military, and refers to a walking with weight on your back – typically in a backpack, a.k.a. a rucksack. The term is now common among the vest-wearing public.
How Does It Work?
Walking with a weighted vest is a low impact exercise that spreads the weight evenly across the body, rather than simply holding free weights. It is recommended that, when starting off, you use weights between 5% and 10% of your body weight for the best effect; otherwise, you risk straining your muscles and/or joints. Once your body has gotten used to this regimen, you may increase the weight by 2% to 5% of your body weight. However, a maximum of 15% is the general rule of thumb, though you may be able to surpass that with experience and a consultation with your physician.
How often should you wear the vest? I recommend two to three times a week, for up to 60 minutes during an exercise session or a maximum of three hours if you are walking. Wearing it all day is very inadvisable, as the extra weight on your back and joints will ultimately pose problems.
Pros
The idea behind wearing a weighted vest is to improve strength, stamina, and overall fitness, as well as potentially lose weight through additional burning of calories. The weighted vest can also benefit those who suffer from osteoporosis. Using the vest can help to build bone density and muscle strength, thus reducing the risk of a fracture, and can positively affect your balance.
As with any new exercise regimen, moderation is key; only by gradually increasing the weight in the vest, and by carefully increasing the length of your workout (walking, calisthenics, etc.), will you realize the greatest benefit. If at any point you feel pain or other uncomfortable side effects, reduce the weights to your former level; if the pain continues, you should see a physician to determine if you may have injured yourself.
Cons
If you suffer from arthritis, particularly in the back and/or knees, proceed carefully. While a weighted vest can help with bone density, muscle strength, and endurance, its use may also aggravate joint pain and strain in the knees, hips and lower back. You may also experience a negative impact on your posture, in which case you probably are carrying too heavy a burden. Either way, discuss with your physician whether a weighted vest – or perhaps some other equipment – may be the best way for you to achieve your exercise goals. A medical professional is always your best resource when it comes to exploring new options.
Either way, discuss with your physician whether a weighted vest – or perhaps some other equipment – may be the best way for you to achieve your exercise goals. A medical professional is always your best resource when it comes to exploring new options.
Dr. Mark Klion is a board-certified Orthopedic Surgeon specializing in Sports Medicine at White Plains Hospital Physician Associates (WPHPA) Orthopedic Surgery in West Harrison. To make an appointment, call 914-849-7897.
Health Matters
The original version of this article was published in Health Matters, a White Plains Hospital publication.
Life-Saving Pregnancy Care at White Plains Hospital
- Details
- Written by: Joanne Wallenstein
- Category: Health
 When Alissa Cheperak’s pregnancy took a turn, the expert care at White Plains Hospital made a life-saving difference for both her and her daughter.
When Alissa Cheperak’s pregnancy took a turn, the expert care at White Plains Hospital made a life-saving difference for both her and her daughter.
When Cheperak discovered she was pregnant, she and her husband, Scott, were ecstatic. The Ossining-based couple were thrilled that their hoped-for timing had worked out, and they knew exactly where to get the best obstetrical care in the region.
As a social worker and a certified case manager at White Plains Hospital, Alissa was already familiar with the world class expertise at the Hospital. She soon found the perfect doctor to see her through the next nine months: OB/GYN Dr. Dana Bryant.
Subtle Symptoms of Major Trouble
Cheperak sailed through her pregnancy, but in July, she began to feel unwell. “One Tuesday night, I woke up with what felt like heartburn” she recalls, “I thought, ‘I’m pregnant, and its common.’”
The next day, the pain persisted. Dr. Bryant suggested an over-the-counter antacid, then a slightly stronger version when the first didn't help. Still, Cheperak’s symptoms worsened.
A Worsening Situation
That Friday, Dr. Bryant got another call from Cheperak. “She described pain wrapping around her rib cage and radiating to her back,” Dr. Bryant says. “I advised her to go to the Emergency Department.” At White Plains Hospital, a chest X-ray and CAT scan ruled out a heart attack and pulmonary embolism, but blood tests revealed something more serious — Cheperak had HELLP syndrome:
• HELLP syndrome (hemolysis, elevated liver enzymes, and low platelet count) is a rare and potentially life-threatening pregnancy complication.
• Affecting fewer than 1% of pregnant women, HELLP can cause dangerously high blood pressure, organ dysfunction, and severe complications; as many as 24% of affected mothers and 34% of babies do not survive.
While Cheperak was seriously ill, she had not yet reached a critical stage. There is only one cure for HELLP; delivery of the baby. In Cheperak’s case, it meant giving birth very early-at 27 weeks.
Dr Bryant didn't rush Cheperak into the operating room. As soon as she was stable, Dr. Bryant performed a C-section. Cheperak’s baby, Claire, entered the world at a mere 1 lb. 10 oz.
“They showed her to us very quickly, because they had to get her hooked up to oxygen,” Cheperak says, overcome with emotion.
Unbeatable Care
Claire spent two long months in White Plains Hospital’s neonatal intensive care unit (NICU). Whether Cheperak’s daughter needed a blood transfusion, or to have her oxygen level increased, someone was on hand to carefully make sure the task was performed.
Like many preemies, Claires health was unstable at first. When, after a month, Claire showed signs of abnormal development of blood vessels of the retina, her care team at White Plains Hospital recommended she be transferred to a hospital where she could receive even more specialized care.
Because White Plains Hospital is a part of the Montefiore Health System, Claire was able to be transferred to Montefiore Medical Center’s Wakefield Campus, where her care would continue within the same network, providing a consistent approach to treatment during a critical time.
A Triumphant Homecoming
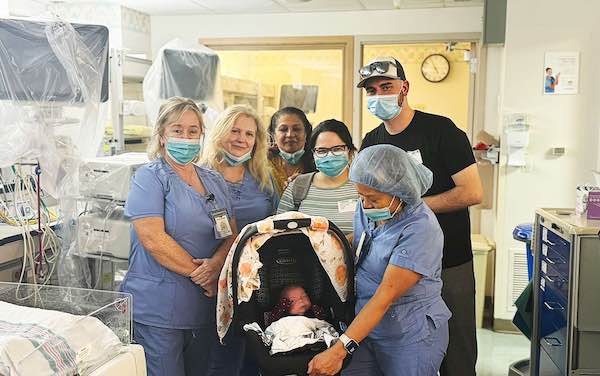
Three months after her birth, Claire was finally ready to go home. Although she requires physical therapy, the nearly 11-month-old has been thriving from the day she arrived home.
Dr. Bryant praises Cheperak for keeping in touch as her condition worsened during the pregnancy. “If your doctor is treating you for a more common symptom, such as heartburn, and it still isn’t getting better, always be willing to speak up,” Dr. Bryant says.
Still, she adds, pregnant women shouldn’t panic if they suffer from heartburn-like sensations. “Most women aren’t going to develop HELLP syndrome,” she stresses. But there’s no better place to seek assistance than at the Hospital, she says: “We have the specialized expertise to quickly assess your situation and help you fully understand whether it is something to be concerned about, or just a normal symptom in a long pregnancy.”
Cheperak and her husband experienced firsthand how even the most carefully planned pregnancies can take unexpected turns. They feel eternally grateful for the care they received at White Plains Hospital when both mother and baby’s lives were on the line.
Learn more about Maternity Services at White Plains Hospital.
Health Matters
The original version of this article was published in Health Matters, a White Plains Hospital publication.
Behind the Trend: Fitness Trackers
- Details
- Written by: Joanne Wallenstein
- Category: Health
 Submitted by Daniel Silovitz, DO, Internal Medicine
Submitted by Daniel Silovitz, DO, Internal Medicine
Fitness bands, smart watches, and even smart rings have flooded the market in recent years.
These popular devices use sensors to help wearers track a variety of health metrics and can be an effective tool to kickstart or monitor your fitness routine, says Dr. Daniel Silovitz, an Internal Medicine Physician with White Plains Hospital Physician Associates.
While step counters are one of the most popular features, modern trackers can monitor more, so wearers should decide what they want to keep track of when shopping for a device.
Some models can be used to keep an eye on important variables in your overall health including:
• Heart rate
• Sleep duration and quality
• Cardiorespiratory fitness levels (helpful for serious workout enthusiasts looking to increase their VO2 max, or maximum oxygen consumption, which it estimates based on your heart rate and distance traveled).
“These devices can be a great way to keep track of your overall health and performance, but they do have limitations,” warns Dr. Silovitz. “They shouldn’t replace going to see your physician.”
Many devices can detect an irregular heartbeat, which may indicate Atrial Fibrillation (AFib), which may have no symptoms and can increase one's risk of stroke and heart failure. Dr. Silovitz also points out that the more you wear these devices, the better they’ll become at synthesizing your personal health data, so consistency is key. Learn more about White Plains Hospital Physician Associates' Internal Medicine and Primary Care Services.
Learn more about White Plains Hospital Physician Associates' Internal Medicine and Primary Care Services.
Dr. Daniel Silovitz is an internal medicine physician at WPHPA of Harrison, specializing in preventive medicine and the management of chronic conditions. To make an appointment, call 914.835.0073.
Health Matters
The original version of this article was published in Health Matters, a White Plains Hospital publication.
Live Long, Stay Strong: 10 Health Commandments
- Details
- Written by: Tony Mathews, MD, MPH.
- Category: Health
 The Blueprint for Living Long and Staying Strong Is Simple—But Not Easy
The Blueprint for Living Long and Staying Strong Is Simple—But Not Easy
Dr. Tony Mathews is an Endocrinologist and Longevity Medicine Specialist with fellowship training in Endocrinology and Preventive Cardiology. He is board certified in Internal Medicine, Endocrinology, Clinical Lipidology, and Obesity Medicine, with over 12 years of experience. For the past three years, he has been honored to serve this community—helping people like you live longer, healthier lives by preventing and managing chronic disease.
Mathews explains, "I have found that we all want more than just a long life—we want a healthy one. We want to feel vital, strong, and full of purpose for as long as possible. This is the concept of healthspan, and it's what drives my personal commitment to wellness."
"These are the 10 Health Commandments I strives toward every day to build a longer, stronger life—principles he hopes will guide you on your own journey."
1. Fuel Wisely: Eat Real Food – Think Apple, Not Apple-Flavored Snack
What you eat becomes who you are. Pick an evidence-informed nutritional style that works for you. Prioritizing whole, unprocessed foods like fruits, vegetables, lean proteins, and whole grains provides the essential nutrients, fiber, and energy needed for optimal function and disease prevention. Support a healthy gut microbiome by including fiber and fermented foods in your diet.
2. Hydrate Intelligently: Drink More Water – Your Body Craves It
Your body is over 60% water. Every cell, tissue, and organ in your body needs water to function properly. Proper hydration aids digestion, nutrient absorption, temperature regulation, waste removal, and even cognitive performance. Make water your go-to beverage throughout the day and aim for 6–8 cups daily. Minimize sugar-sweetened beverages.
3. Strengthen Your Heart & Lungs: Keep the Engine Running
Move as much as possible each day. Aim for at least 150 minutes of moderate-intensity aerobic exercise—like brisk walking, cycling, or swimming—or 75 minutes of vigorous-intensity activity per week. Include high-intensity interval training, especially when you're short on time.
4. Build & Maintain Muscle: Your Foundation to Carry You Through Life
You can lose up to 40% of your muscle mass between ages 30 and 70. It’s easier to build muscle today than it will be tomorrow. Incorporate resistance training 2–3 times a week to build muscle today and maintain it tomorrow—your future mobility and independence depend on it.
5. Champion Rest and Recovery: Sleep Is Your Body’s Reset
Sleep is not a luxury; it’s a biological necessity. During sleep, your body undergoes critical repair processes, consolidates memories, and regulates hormones. Aim for 7–8 hours of quality sleep each night. Sleep consistency is just as important as duration, so try to go to bed and wake up at the same time every day.
6. Do No Harm: Avoid Known Toxins
Smoking remains a leading cause of preventable death and disease. If you smoke, there are many resources to help you quit. Similarly, while moderate alcohol consumption may be acceptable for some, excessive intake can harm your liver, brain, and significantly increase your risk of cancer.
7. Cultivate Stress Resilience: Teach Yourself to Bounce Back
Chronic stress can negatively affect nearly every system in your body. While stressors are an inevitable part of life, developing resilience helps you adapt and recover. Practices like mindfulness, deep breathing, journaling, and spending time on hobbies can significantly boost your ability to cope effectively.
8. Nurture Your Mind: It Is Your Greatest Asset
Your mental health is deeply linked to your physical health. Take proactive steps to care for your emotional and psychological well-being. This includes practicing self-compassion, acknowledging your feelings without judgment, and engaging in activities that bring you joy. Keep your mind sharp with new skills, creative pursuits, and meaningful conversation—and recognize when professional support may be helpful.
9. Connect for Longevity: Forge Strong Social Bonds
Humans are wired for connection. Meaningful relationships offer emotional support, reduce loneliness, and can even improve physical health and longevity. Make an effort to nurture existing relationships and cultivate new ones by joining groups, volunteering, or simply reaching out to friends and family.
10. Reconnect with Nature: Find Your Outdoor Sanctuary
Spending time outdoors has been shown to reduce stress, improve mood, and increase physical activity. Whether it’s a walk in a local park, tending a small garden, or taking a weekend hike, make time to connect with the natural world. Even short, regular exposure to nature offers real benefits.
Let’s Build Your Healthspan Together
Ready to take the next step on your path to a longer, stronger life? Discover proactive health and longevity care with Dr. Tony Mathews and the team at Sequoia Medical 360—Your Partner In Proactive Health.
Dr. Tony Mathews is a Dual Fellowship-Trained, Quadruple Board-Certified Endocrinologist and Longevity Medicine Specialist with over 12 years of experience, who has spent the past 3 years serving our local community.
Sequoia Medical 360 is a Concierge Medical Practice based out of Bronxville and serves the Westchester community.
Call 914-292-0300 today and take the first step toward a healthier, stronger future—right here at home.
Finding Your Perfect Match: How to Choose an OB-GYN for Your Pregnancy Journey
- Details
- Written by: Joanne Wallenstein
- Category: Health
 Submitted by Dr. Nabil Khoury, OB/GYN at White Plains Hospital
Submitted by Dr. Nabil Khoury, OB/GYN at White Plains Hospital
Choosing an OB-GYN for your pregnancy journey is an important step for new parents.
“The birth process is a very personal and private matter, so patients need someone who is knowledgeable and will build trust with the family,” says Dr. Nabil Khoury, an OB-GYN with White Plains Hospital Physician Associates who has been practicing in the region for more than 27 years. He offers this advice:
Ask around
Talk to a trusted healthcare provider whom you respect to see if they have any recommendations. Family and/or friends who have had a positive experience with their OB-GYN can be another avenue to finding the right provider. OB-GYN physicians who deliver at White Plains Hospital can also be found online at wphospital.org.
Look for a provider who is reassuring
“With any pregnancy, it’s normal to feel fear of the unknown. An important part of your OB-GYN’s role is to reassure patients, educate them and carry them through the whole process,” Dr. Khoury says.
Seek a collaborative experience
Dr. Khoury feels the team approach at White Plains Hospital, which offers Maternal-Fetal Medicine (MFM) physicians who work in conjunction with your own OB-GYN, is a real benefit for patients. By collaborating, the team can conduct genetic testing in the preconception period and throughout the pregnancy. They also have the ability to treat high-risk patients or complicated pregnancies, working towards a healthy outcome for both mom and baby.
Dr. Khoury and his team are also able to access other services from the Hospital if needed. For example, if a woman is anemic during pregnancy and needs an iron infusion, Dr. Khoury’s office will call the hematology department at the Hospital and and make sure that she will be seen in a timely fashion. “If a problem arises, we take care of it and put the mother in touch with the specialist she needs to see. If a patient calls us with a need for an appointment or a question, we are accessible and can facilitate that appointment as soon as possible,” he explains.
Learn more about the Maternal Healthcare Services available at White Plains Hospital.
Dr. Nabil Khoury is an OB-GYN with White Plains Hospital Physician Associates who has been practicing in the region for more than 27 years. To make an appointment, call 914-328-8444.
 Health Matters
Health Matters
The original version of this article was published in Health Matters, a White Plains Hospital publication.






