White Plains Hospital Expands Its Team-Based Approach to Multiple Sclerosis Care
- Details
- Written by: Joanne Wallenstein
- Category: Health
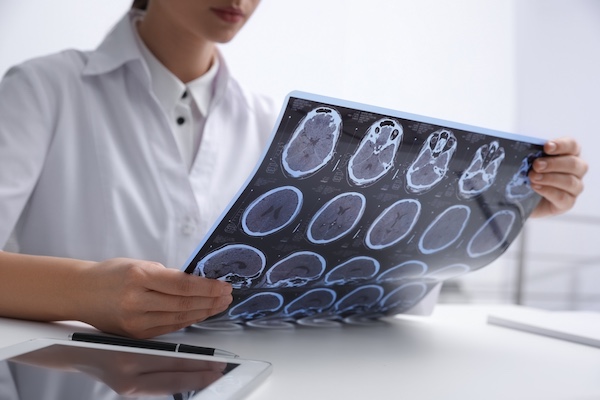 Cases of multiple sclerosis (MS), a chronic autoimmune disease affecting the brain, spinal cord and optic nerves (the nerves that transmit signals from the eyes to the brain), are on the rise in the United States, impacting nearly 1 million people nationwide. For many patients, a diagnosis can feel overwhelming and raise questions such as:
Cases of multiple sclerosis (MS), a chronic autoimmune disease affecting the brain, spinal cord and optic nerves (the nerves that transmit signals from the eyes to the brain), are on the rise in the United States, impacting nearly 1 million people nationwide. For many patients, a diagnosis can feel overwhelming and raise questions such as:
• What does this mean for my future?
• Will I be able to work or maintain my lifestyle?
• What treatments are available?
At White Plains Hospital, patients have expanded access to specialized, comprehensive MS care close to home at its Multiple Sclerosis Center, which has been based at the Hospital since 2004. Over the years, the Center has continued to grow and evolve, expanding its team of dedicated MS specialists and broadening its treatments and resources for patients.
White Plains Hospital is the only healthcare organization in Westchester designated as a Center for Comprehensive MS Care through the National Multiple Sclerosis Society’s Partners in MS Care program.
Coordinated Care Led by an MS Specialist
The Center is led by Dr. Ute Traugott, an internationally recognized MS specialist with more than 40 years of experience. She specializes exclusively in MS and related neuroimmunologic disorders and serves as Program Director, guiding a highly coordinated, multidisciplinary team.
“Certification by the National Multiple Sclerosis Society is very important,” Dr. Traugott says, “as it assures patients that there is a highly qualified group of specialists forming a treatment team to provide the best and up-to-date comprehensive care.”
The program recently expanded with Dr. Mark Tullman as Associate Director, who brings two decades of MS-focused experience, and Dr. Samantha Epstein, a neurologist with additional specialized training in neuroimmunology, enhancing patient access to expert care across the disease spectrum.
A Team-Based, Patient-Focused Model
With a team of experts working together under one roof, patients at White Plains Hospital’s MS Center experience care that is coordinated, comprehensive and supports every aspect of living with MS. Key benefits include:
• Expert evaluation and diagnosis: Accurate diagnosis using MRI, blood tests, and spinal fluid analysis, distinguishing MS from related conditions.
• Personalized treatment plans: Disease-modifying therapies tailored to reduce relapses and slow disease progression. Pharmacologic and nonpharmacologic therapies to alleviate the daily symptoms of MS often play an integral part in patient care.
• Access to advanced therapies: At this time, over 20 FDA-approved treatments are available. In addition, new medications are in clinical trials targeting inflammation and myelin repair.
• Integrated specialty services: Physical and occupational therapy, urologic care, pain management, and mental health support.
In addition, the team meets regularly with colleagues specializing in neuroradiology to review complex cases, ensuring that every patient receives the most appropriate care.
Understanding MS: Symptoms and Diagnosis
“In patients with MS, the immune system attacks and damages the central nervous system — the brain, spinal cord and optic nerves,” says Dr. Epstein. “That damage can result in weakness, numbness and tingling, vision problems, fatigue, and difficulties with coordination and balance.”
“There is no single diagnostic test,” Dr. Epstein adds. “MS is diagnosed through a combination of clinical history, neurologic examination, imaging, blood tests, and, if necessary, evaluation of spinal fluid.”
Specialized Care for Complex Conditions
Drs. Epstein, Traugott and Tullman also treat patients with rare autoimmune neurologic disorders such as:
• Neuromyelitis optica spectrum disorder
• Myelin oligodendrocyte glycoprotein (MOG)-associated disease (MOGAD)
“These conditions can resemble MS but require distinct approaches,” Dr. Tullman explains. “My focus complements Dr. Traugott’s leadership to care for patients at every stage — from newly diagnosed to long-term management.”
“We work closely with rehabilitation specialists and other subspecialists to address the full spectrum of patient needs,” Dr. Traugott says.
“Our goal is not just excellent clinical care, but an exceptional patient experience,” adds Dr. Tullman.
With the addition of new physicians and ongoing advances in treatment and research, the Center remains committed to providing patients with expert, coordinated care at every stage of their MS journey.
Learn more about Multiple Sclerosis Services at White Plains Hospital.
This article originally appeared on Health Matters, a White Plains Hospital publication.
The HPV Vaccine: What Every Parent Should Know
- Details
- Written by: Joanne Wallenstein
- Category: Health
 By the time children reach 11 or 12 years old, they have received many routine vaccinations required for school. However, there is one vaccine that may not be required — yet it is one of the most powerful cancer-prevention tools we have: the HPV vaccine.
By the time children reach 11 or 12 years old, they have received many routine vaccinations required for school. However, there is one vaccine that may not be required — yet it is one of the most powerful cancer-prevention tools we have: the HPV vaccine.
What Is HPV?
Human papillomavirus (HPV) is not a single virus — it is a group of more than 150 related viruses that infect the skin and the moist surfaces of the body, including:
- The cervix
- Vagina and vulva
- Penis
- Anus and rectum
- Mouth and throat (including the base of the tongue and tonsils)
HPV is the most common sexually transmitted infection in the United States, with nearly all sexually active males and females getting exposed to the virus at some point in their lives.
While many infections clear on their own, certain strains can persist and lead to genital warts as well as a variety of cancers. There is currently no cure for HPV infection. Vaccination is our best and only tool to prevent many of these cancers before they start.
Why the HPV Vaccine Matters So Much
The HPV vaccine is unique because it is a cancer-prevention vaccine since there is no cure for HPV.
According to the American College of Obstetricians and Gynecologists, the vaccine demonstrates greater than 99% effectiveness in preventing when given before exposure. Two doses, given six months apart, are recommended for all children ages 9-14. Three doses are recommended for those ages 15-26, and some adults up to age 45 may choose vaccination after discussing risk with their physician.
The vaccine:
- Prevents the majority of cervical cancers
- Protects against several other HPV-related cancers in both males and females
- Prevents most genital warts
- Is safe and FDA-approved
Addressing Common Concerns
Many parents understandably have questions.
“My child isn’t sexually active. Why vaccinate now?”
- The vaccine works best before exposure to HPV.
- The immune response is stronger at ages 11–12 than later in life.
- Waiting until sexual activity begins reduces the vaccine’s protective benefit.
“Isn’t HPV only a concern for girls?”
- HPV causes cancers in both males and females.
- Boys can develop throat, anal, and penile cancers linked to HPV.
- Vaccinating boys also helps reduce transmission overall.
 The HPV vaccine is safe, effective, and a powerful tool for preventive health, and your child’s pediatrician can help guide you in making it part of a personalized plan for lifelong health.
The HPV vaccine is safe, effective, and a powerful tool for preventive health, and your child’s pediatrician can help guide you in making it part of a personalized plan for lifelong health.
Dr. Gilbert Herzberg is a pediatrician at White Plains Hospital Physician Associates and sees patients at 750 White Plains Road in Scarsdale. To make an appointment, call 914-974-5437.
Health Matters
The original version of this article was published in Health Matters, a White Plains Hospital publication.
What Parents Can Expect From Fetal Echocardiography
- Details
- Written by: Joanne Wallenstein
- Category: Health
 Pregnancy is full of excitement – and sometimes worry. If an ultrasound raises questions about a baby’s heart, or there’s a known risk factor, expectant mothers may be referred for a fetal echocardiogram. While this can feel intimidating, it is often a reassuring step that helps families understand their baby’s health and plan for the future.
Pregnancy is full of excitement – and sometimes worry. If an ultrasound raises questions about a baby’s heart, or there’s a known risk factor, expectant mothers may be referred for a fetal echocardiogram. While this can feel intimidating, it is often a reassuring step that helps families understand their baby’s health and plan for the future.
A fetal echocardiogram is a specialized ultrasound that examines a baby’s heart before birth, explains Dr. Marise D’Souza, a pediatric cardiologist at the Children’s Hospital at Montefiore who sees patients at White Plains Hospital’s Pediatric Specialty Center. It provides detailed images that show how the heart is structured and how it’s functioning while the baby is in the womb.
Why a Fetal Echocardiogram May Be Recommended
Most women receive a routine anatomy ultrasound during pregnancy. A fetal echocardiogram is only recommended when there’s a reason to take a closer look, such as:
• An abnormal finding on routine ultrasound, such as one side of the heart or a valve looking smaller than expected
• Family history of congenital heart disease
• Maternal conditions like lupus or Sjögren’s syndrome
• Certain medications or exposures, or certain medical conditions such as diabetes or autoimmune conditions
• Difficulty visualizing the heart clearly on a standard ultrasound
The good news is that most fetal echocardiograms show the heart is developing normally, which can bring enormous relief.
What Happens During the Exam
Fetal echocardiography is noninvasive and safe for both parent and baby. During the exam, the cardiologist evaluates:
• Heart chambers
• Valves
• Blood vessels
• Heart rhythm
Parents also have time to ask questions and get clear, compassionate explanations.
Dr. D’Souza emphasizes that the goal isn’t just diagnosis, it’s preparation. Early detection allows families and care teams to plan for the best possible outcome.
Detecting a heart condition before birth gives families time to learn about the condition in advance, explore treatment options, and plan for delivery in the safest setting if specialized care or surgery are needed after the baby’s birth.
Care Close to Home
Having access to fetal echocardiography locally helps reduce stress. For more complex cases, providers can coordinate care seamlessly within the Montefiore Health System, ensuring babies receive advanced care while families stay close to home.
Whether the exam rules out serious heart disease or identifies a condition needing treatment, the goal is the same: supporting babies, children, and families with expert care, clear communication, and compassion. Dr. Marise D’Souza is pediatric cardiologist at the Children’s Hospital at Montefiore and sees patients at White Plains Hospital’s Pediatric Specialty Center. To make an appointment, call 914.849.5437.
Dr. Marise D’Souza is pediatric cardiologist at the Children’s Hospital at Montefiore and sees patients at White Plains Hospital’s Pediatric Specialty Center. To make an appointment, call 914.849.5437.
The original version of this article was published in Health Matters, a White Plains Hospital publication.
Coronary Artery Disease: A Silent Threat to Heart Health
- Details
- Written by: Joanne Wallenstein
- Category: Health
 Submitted by Gregory Pontone, MD, MBA, Cardiology at White Plains Hospital
Submitted by Gregory Pontone, MD, MBA, Cardiology at White Plains Hospital
Coronary artery disease (CAD), also known as atherosclerosis, is the most common form of heart disease. According to the CDC, it claims the lives of an estimated 375,000 Americans each year.
Often described as “hardening of the arteries,” CAD develops slowly, sometimes over decades. It occurs when plaque continues to accumulate inside the arteries that supply blood to the heart, narrowing them and limiting blood flow.
Because this buildup happens gradually, the risk of CAD increases with age. A November 2025 report published in the American Heart Association’s Circulation journal found that adults age 75 and older account for up to 40% of hospitalizations for acute coronary syndrome (ACS). Often the result of CAD, ACS occurs when plaque suddenly ruptures, forming a clot that blocks blood flow and can trigger a heart attack.
Hidden Dangers
One of the most dangerous aspects of CAD is how quietly it can develop. The disease may be present for years—in rare cases, even in children—without causing noticeable symptoms. When symptoms do appear, such as chest pain or shortness of breath, they often don’t emerge until someone is in their 60s or later.
Even then, symptoms can be subtle or intermittent and may be mistaken for other conditions, including anxiety, allergies, emphysema, or even a collapsed lung. Unfortunately, for many people, the first sign of CAD is a sudden heart attack. This is why regular medical checkups are so important.
Who Is at Risk?
Several risk factors for CAD can be modified or managed.
These include:
• High blood pressure
• Diabetes
• Smoking
• Physical inactivity
Family history also matters, particularly if a parent or sibling has had CAD. Men are generally at higher risk, although a woman’s risk increases after menopause due to hormonal changes.
How CAD Is Detected
Assessing your risk for CAD can be straightforward. A routine blood test can reveal diabetes, plaque-related proteins, and abnormal levels of low-density lipoprotein (LDL, the “bad” cholesterol) and high-density lipoprotein (HCL, the “good” cholesterol).
Noninvasive tests such as chest X-rays, electrocardiograms (EKGs), and cardiac positron emission tomography (PET) scans of the heart can also reveal CAD.
Another valuable tool is a coronary calcium score, a specialized CT scan that measures calcification in the arteries to estimate your risk of a heart attack over the next 10 years:
• Mild risk: 1–100
• Moderate risk: 100–300
• Severe risk: Above 300
A severe score—sometimes reaching several hundred—signals the need for prompt action, including major lifestyle changes, medications, additional tests, and possibly stenting or a bypass.
Next Steps
If a person’s case of CAD is found to be especially concerning, there are several prudent treatment options. These can range from taking medications to undergoing surgery. If you are concerned that you may be at risk for, or already have, CAD, ask your doctor to perform an EKG, bloodwork, and/or a calcium score test. Early detection can make a life-saving difference.
 Dr. Gregory Pontone is the Acting Chief of the Cardiology Department at White Plains Hospital. He is a noninvasive cardiologist, and also serves as the Associate Medical Director of Ambulatory Quality & Physician Services. To make an appointment, call 914-849-4800.
Dr. Gregory Pontone is the Acting Chief of the Cardiology Department at White Plains Hospital. He is a noninvasive cardiologist, and also serves as the Associate Medical Director of Ambulatory Quality & Physician Services. To make an appointment, call 914-849-4800.
Health Matters
The original version of this article was published in Health Matters, a White Plains Hospital publication.
Breathing Easier by Staying Ahead of Pneumonia
- Details
- Written by: Joanne Wallenstein
- Category: Health
 (Submitted by Dr. Christopher Robles, Family Medicine, Primary Care)
(Submitted by Dr. Christopher Robles, Family Medicine, Primary Care)
Most of us have heard of pneumonia, but do we really know what it is and, more importantly, how to protect ourselves against it?
Pneumonia is an infection of the lower respiratory tract that causes the lungs’ air sacs to become inflamed and fill with fluid, making it harder to breathe. Symptoms include cough, fever, chills, and shortness of breath.
How serious is pneumonia? According to the latest available statistics, approximately 1.5 million American adults are diagnosed with it each year, leading to around 1 million hospitalizations and 50,000 deaths.
The most prevalent form of pneumonia—estimated to account for as many as 50% of all cases—is viral. The influenza virus is one of the most typical causes in adults, while respiratory syncytial virus (RSV) is the most common cause in young children. Fortunately, viral pneumonia often can clear up on its own.
The second most frequent is bacterial pneumonia, which can be more severe and usually requires antibiotic treatment.
Pneumonia is often believed to be an “older person’s disease.” Although adults aged 65 and older are at a higher risk due to weakening immune systems and, in many cases, having medical conditions like COPD, asthma, and chronic kidney or liver disease. Children aged 0-2 are equally susceptible due to their still-developing immune systems.
This is not to say that people outside of those age groups cannot get pneumonia; in fact, everyone can get it. Exacerbating factors include:
• Pre-existing medical conditions like those listed above.
• Health-compromising behaviors like smoking or substance abuse, including alcohol, marijuana, cocaine, and opioids.
• Your environment. Long-term exposure to contaminated water, surfaces, and polluted air can leave you more susceptible to disease-causing germs, as can being in a situation where infected people are coughing, sneezing, or even breathing.
Reducing Your Risk
You can contract pneumonia at any time of the year, making the need to protect yourself even more important. My tips for reducing your risk:
Get vaccinated. Many people are unaware there’s a vaccine for Streptococcus pneumoniae—the bacteria that can cause pneumonia as well as meningitis and various ear and sinus infections. It has been estimated that a vaccination can significantly reduce the risk of developing the disease.
• The CDC recommends pneumococcal vaccination for children younger than 5 and adults aged 50 and older (the latter was lowered in 2024 from 65 and older).
• As with the flu vaccine, the pneumococcal vaccine is covered by most insurance. A single dose usually provides lifelong protection for adults.
Follow healthy habits.
• Wash your hands frequently.
• Disinfect frequently touched surfaces.
• Eat a healthy diet, get rest and regular exercise.
• Try to avoid people who are sick.
• Avoid smoking. Not only should you not smoke, you should also limit your exposure to secondhand smoke.
Finally, continue to manage your other chronic medical conditions. This includes regular monitoring of those conditions and being extra cautious when dealing with any additional respiratory symptoms.
Pneumonia is serious but often preventable. Know the signs, act quickly if symptoms appear, and take simple steps like vaccination and good hygiene to protect yourself. Early action can make all the difference; breathe easier by staying informed. Dr. Christopher Robles is a family medicine and primary care physician, seeing patients at the Somers and White Plains locations. To make an appointment, please call 914-849-7075.
Dr. Christopher Robles is a family medicine and primary care physician, seeing patients at the Somers and White Plains locations. To make an appointment, please call 914-849-7075.
Health Matters
The original version of this article was published in Health Matters, a White Plains Hospital publication.











