Advanced Care for Kids, Close to Home
- Details
- Written by: Joanne Wallenstein
- Category: Health
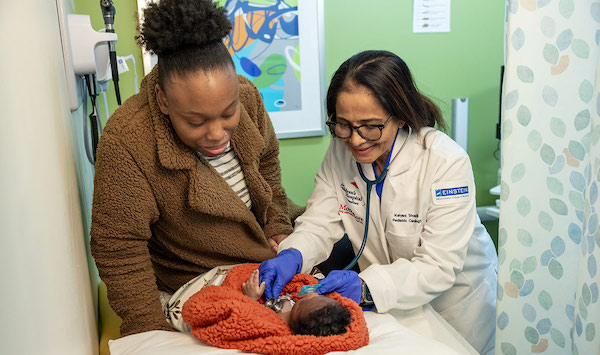 (This article was submitted by White Plains Hospital)
(This article was submitted by White Plains Hospital)
Living in Westchester County brings many benefits, including good schools, recreational spaces, cultural offerings, and more. Improved access to pediatric subspecialty care is yet another advantage for Westchester families. The recent expansion of the White Plains Hospital Pediatric Specialty Center—a partnership between White Plains Hospital and the renowned Children’s Hospital at Montefiore Einstein (CHAM)—has brought to the region convenient pediatric subspecialty care that parents elsewhere have to travel far and wide to access.
“With only approximately 400 pediatric rheumatologists in the U.S., very few families have access to a pediatric rheumatologist right in their community,” says Dr. Michael Cabana, Physician-in-Chief at CHAM and Chair of Pediatrics at Albert Einstein College of Medicine. That won’t be an issue here in Westchester.
“We are pleased to bring even more renowned pediatric subspecialists to care for our youngest patients close to home at White Plains Hospital,” adds Frances Bordoni, Executive Vice President for Ambulatory and Physician Services and Business Development at White Plains Hospital. “Removing the need to travel to receive high-quality care for their children saves time and peace of mind for busy parents in the Hudson Valley, allowing them to focus on what matters most.”
With the expansion, seven additional providers are available at the White Plains Hospital Pediatric Specialty Center, which is now home to 23 pediatric subspecialists from Montefiore. The physicians see patients at the Center’s offices at 33 Davis Avenue in White Plains, at Scarsdale Medical Group in Harrison and at the Hospital’s Center for Advanced Medicine & Surgery.
They specialize in a range of pediatric care including:
• Adolescent medicine
• Pediatric cardiology
• Endocrinology (including juvenile diabetes and bone health/growth care)
• Gastroenterology
• Nephrology
• Orthopedics
• Otolaryngology
• Pulmonology
• Rheumatology
• Surgery
Highly trained physicians of this kind are in short supply nationwide. “It’s ironic—we have better therapies than ever for kids who need specialty care, yet many people don’t have access to a subspecialist,” explains Dr. Cabana. “That’s why this Center is really important.” Pediatric GI specialists, for instance, are experts in treating irritable bowel diseases like Crohn’s disease and ulcerative colitis. Urologists can address conditions such as prenatal hydronephrosis, or the swelling of a kidney in a fetus or infant. Pulmonologists offer long-term care for children with asthma.
“We’ve got everything covered,” Dr. Cabana says. “There are so many things we can do in pediatric care now that we couldn’t do when I trained as a pediatrician 30 years ago. Our job is making sure those therapies are accessible and that kids get the very best care, at the right time, as conveniently as possible.”
In fact, the outpatient treatments provided at the Pediatric Specialty Center are so successful, they are able to prevent most pediatric patients from needing hospital admission. “We can use great new medicines like monoclonal antibodies, which have been available to adults for the past two decades, to help prevent flare-ups and hospitalizations for kids with chronic diseases,” Dr. Cabana says.
If a child’s condition gets to the point where they require hospitalization, they benefit from the seamless coordination of care between White Plains Hospital and CHAM, which ensures continuity and expertise at every step. This collaborative approach enables patients access to CHAM’s Pediatric Heart Center, a world leader in advanced cardiovascular care for patients with congenital heart diseases, as well as its renowned pediatric surgery services and comprehensive program for children with kidney problems, including New York state’s first dedicated pediatric dialysis facility.
Dr. Cabana notes that the Pediatric Specialty Center is the latest benefit of the partnership between
White Plains Hospital and Montefiore
“Many of our physicians actually live in Westchester, so the local connection is very strong,” he adds. “I am so proud of these providers, and now, with even more physicians we can care for a greater number of patients in Westchester and the lower Hudson Valley.”
To make an appointment at the White Plains Hospital Pediatric Specialty Center, call 914-849-KIDS (5437) or view the list of doctors at the White Plains Hospital Pediatric Specialty Center.
Health Matters
The original version of this article was published in Health Matters, a White Plains Hospital publication.
Over 500 Runners Participate in the 55th Annual 15K & 4 Mile Run
- Details
- Written by: Sharon Higgins
- Category: Health
 On Sunday, April 6th over 500 runners took their marks to participate in Scarsdale’s 55th Annual 15 Kilometer and 4 Mile Road Races. The races were organized by the Village’s Department of Parks, Recreation and Conservation. Superintendent Brian Gray was extremely happy with the turn out and smooth running of the races by his staff and community volunteers as well as the Scarsdale Police Department, Scarsdale Fire Department, Scarsdale Volunteer Ambulance Corp and Scarsdale Department of Public Works, who all worked in various roles to support this event.
On Sunday, April 6th over 500 runners took their marks to participate in Scarsdale’s 55th Annual 15 Kilometer and 4 Mile Road Races. The races were organized by the Village’s Department of Parks, Recreation and Conservation. Superintendent Brian Gray was extremely happy with the turn out and smooth running of the races by his staff and community volunteers as well as the Scarsdale Police Department, Scarsdale Fire Department, Scarsdale Volunteer Ambulance Corp and Scarsdale Department of Public Works, who all worked in various roles to support this event.
Mr. Gray commented: “as I left my house it was pouring rain and I was questioning whether or not runners would turn  up. Thankfully, as I arrived in Scarsdale and was doing my pre-course drive-through, the rain slowed and temps rose to optimal conditions for running. After reflecting on Sunday’s event, I look back on the 18 years I have been the Race Director of the Annual Road Races. One of the most satisfying things to witness is the community support of residents cheering runners on with handmade signs and banners, and in a few cases, setting up water stops for runners along the course.”
up. Thankfully, as I arrived in Scarsdale and was doing my pre-course drive-through, the rain slowed and temps rose to optimal conditions for running. After reflecting on Sunday’s event, I look back on the 18 years I have been the Race Director of the Annual Road Races. One of the most satisfying things to witness is the community support of residents cheering runners on with handmade signs and banners, and in a few cases, setting up water stops for runners along the course.”
The weather outside was a cool 45 degrees and overcast. The air was a bit damp but besides that the conditions for the races were ideal. This year, there were a total of 597 registrations with 521 (87%) showing. This is up slightly from last year with 588 registrations and 487 (83%) showing. There was a healthy spread of veterans and newcomers. I spoke with participants as they got ready for the race, collected their numbers, and grabbed water or a snack. Many indicated that they have been participating in this particular race for years while others said it was their first road race ever. Some were serious runners and others were simply there for a “fun run” and admitted to walking hills if that is what it took to finish.
At a little before 9:15am, at the corner of Harcourt and Hampton Roads, the 4 Mile registered runners of all ages— including parents pushing their children in jogger strollers— lined up to start the race. Instructions and well wishes were given to the runners over a microphone by a Scarsdale Park, Recreation and  Conservation representative. The air horn sounded and they were off.
Conservation representative. The air horn sounded and they were off.
At this time, the 15K runners were making their way to their race starting line, just feet away from the entrance to the high school on Brewster Road. Announcements on the course layout supported by lawn signs and finish line were given as well as a quick address from Scarsdale Mayor Justin Arest. Right before the air horn blew at 9:30am, a PRC representative gave a final call to be careful of possible wet patches even though the streets had been cleaned by the town and therefore they should “run their personal best; it is perfect weather for it!”.
Runners in both races ran loops marked with lawn signs indicating race directions in the Fox Meadow and Greenacres neighborhoods with hills and flats scattered throughout the courses. Police blocked the race roads from traffic to ensure the safety of the participants and a police motorcycle escorted the last runners. Water tables were set up along the course manned by volunteers and PRC representatives.
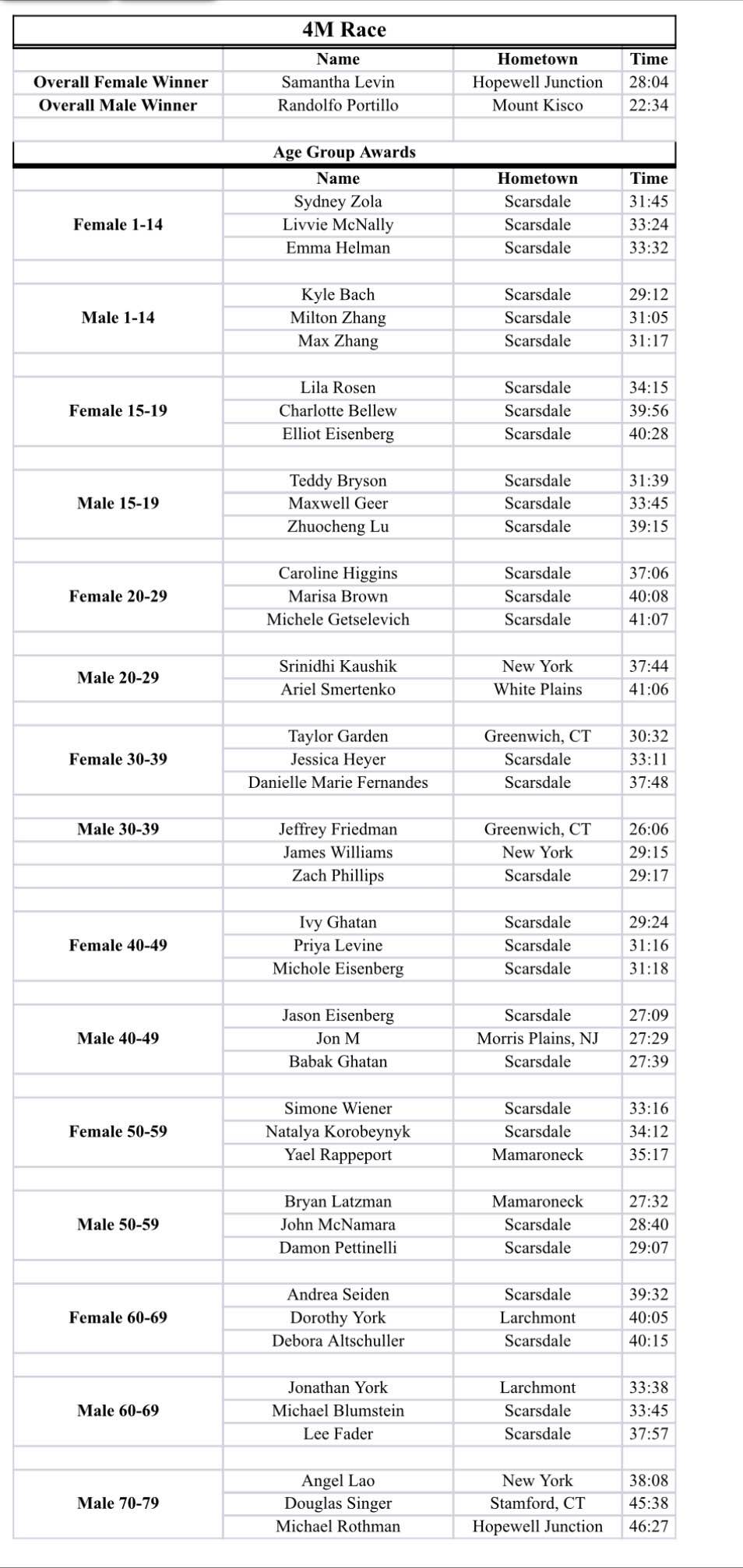
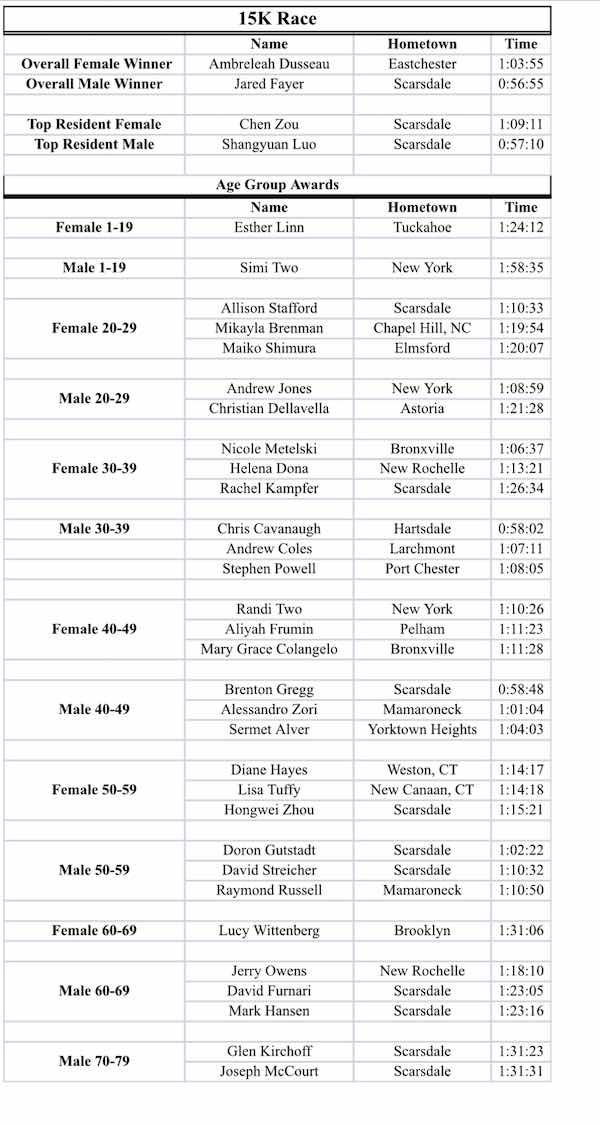
 In twenty two minutes thirty four seconds, with spectators cheering him on, Randolfo Portillo of Mount Kisco was the first runner of the 4 Mile Race to cross the finish line set up a little more than halfway around the Scarsdale High School track. Cheers continued from friends and family members as participants ran across the finish line for the next 55 minutes. Runners made their way into the high school circle. The Scarsdale Fire Department had set up a ladder truck bearing a gigantic American flag. Participants ran under the flag on their way to the last stretch of the course around 2/3 of the track with the finish line set up by the bleachers. With most of the 4 Mile runners through, the crowd roared for Jared Fayer, a Scarsdale resident, who finished first in the 15K race with an impressive time of 56 minutes and 55 seconds.
In twenty two minutes thirty four seconds, with spectators cheering him on, Randolfo Portillo of Mount Kisco was the first runner of the 4 Mile Race to cross the finish line set up a little more than halfway around the Scarsdale High School track. Cheers continued from friends and family members as participants ran across the finish line for the next 55 minutes. Runners made their way into the high school circle. The Scarsdale Fire Department had set up a ladder truck bearing a gigantic American flag. Participants ran under the flag on their way to the last stretch of the course around 2/3 of the track with the finish line set up by the bleachers. With most of the 4 Mile runners through, the crowd roared for Jared Fayer, a Scarsdale resident, who finished first in the 15K race with an impressive time of 56 minutes and 55 seconds.
Names and times of all winners in each category for each race are listed in the tables below. Congratulations to all the participants and workers of the event. You are all winners!
A Troubling Trend: Stroke Risk in Young Populations
- Details
- Written by: Joanne Wallenstein
- Category: Health
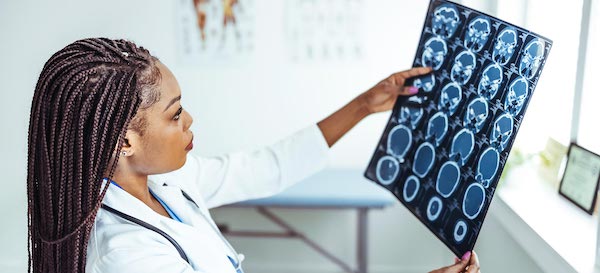 (Submitted by Dr. Paul Lleva, MD, Neurology at White Plains Hospital)
(Submitted by Dr. Paul Lleva, MD, Neurology at White Plains Hospital)
After shoveling and carrying heavy groceries, a young woman begins to feel dizzy and unsteady. Noticing one eyelid drooping, she heads to the emergency room. Although her CAT scan appears normal, further tests reveal high blood pressure and a blood-vessel blockage caused by a dissected carotid artery. At just 30 years old, she has suffered a stroke.
This recent case, shared by Dr. Paul Lleva, Director of Stroke Services at White Plains Hospital, highlights a growing concern: the rise in stroke rates among younger individuals.
Nearly 800,000 people have strokes in the United States each year. Most occur after the age of 65, but new data suggests one in seven strokes now occur in adults ages 15 to 49. Furthermore, a report from the Centers for Disease Control shows a concerning 15% rise in strokes among adults under 65 over the past decade, while rates for seniors have remained consistent.
“Many health issues are now occurring at a younger age,” says Dr. Ivo Bach, a Neuro-Endovascular Surgeon and Vascular Neurologist with White Plains Hospital Physicians Associates. Young adults have seen recent rises in obesity, high blood pressure, and diabetes, as well as opioid use — all factors experts say likely correlate to the rise of strokes. “A lot of it boils down to lifestyle — health, exercise, diet,” says Dr. Bach. “Those are modifiable risks we can alter or stop to prevent strokes.”
For patients under 50 who are active, trauma is often the cause of the stroke. Sports injuries and accidents that twist or jerk the neck can tear arteries, creating clots that may break off and block blood flow to the brain. Updated protocols for such injuries have also led to increased identification of stroke.
“In the old days, if someone was playing football, how many of those kids were brought to the hospital after neck injury? How many were scanned with vascular imaging? Probably only a few,” Dr. Lleva explains. “Now, more patients are screened following traumatic incidents and that is one reason why we are seeing this trend.”
White Plains Hospital offers the most comprehensive treatments for patients of all ages suffering a stroke. In the cases of a dissected carotid artery, the specialized team performs advanced stenting procedures to restore blood flow. During an ischemic stroke, where a blood clot interrupts blood flow to the brain, the team performs a mechanical thrombectomy. Time is of the essence, as with each passing minute, about 1.9 million brain cells die, increasing risk for impairment, disability, and death. Dr. Paul Eugene P. Lleva
Dr. Paul Eugene P. Lleva
A mechanical thrombectomy is the gold standard for stroke care and is a minimally invasive procedure in which specialty trained physicians thread a catheter to the brain to remove clots. Last year, White Plains Hospital received a Thrombectomy-Capable certification from The Joint Commission, indicating that it meets rigorous standards for performing endovascular thrombectomy and providing post-procedural care. “It means if you come to the Hospital for stroke care, we have a specialized team which is ready 24/7 to provide the most advanced care,” Dr. Bach says.
Learn more about Stroke Care at White Plains Hospital.
Dr. Paul Eugene P. Lleva is the Director of Stroke Services at White Plains Hospital. To make an appointment, call 914-849-4800. Dr. Ivo BachDr. Ivo Bach is a neuro-endovascular surgeon and vascular neurologist with White Plains Hospital Physician Associates (WPHPA), with offices in our WPHPA Neurosurgery & Neuro-Endovascular Surgery location in White Plains. To make an appointment, call 914.849.5300.
Dr. Ivo BachDr. Ivo Bach is a neuro-endovascular surgeon and vascular neurologist with White Plains Hospital Physician Associates (WPHPA), with offices in our WPHPA Neurosurgery & Neuro-Endovascular Surgery location in White Plains. To make an appointment, call 914.849.5300.
Health Matters
The original version of this article was published in Health Matters, a White Plains Hospital publication.
The Link Between Alcohol and Several Types of Cancer
- Details
- Written by: Joanne Wallenstein
- Category: Health

(Submitted by Dr. Yael Sadan Zack, Hematology and Medical Oncology, White Plains Hospital)
Most of us are aware that smoking is a leading cause of cancer, and that drinking alcohol can also have deleterious effects on our health. But the U.S. Surgeon General recently published an advisory underscoring that alcohol consumption is the third leading preventable cause of cancer in the U.S., after tobacco and obesity – and increases the risk for at least seven types of cancer.
While scientific evidence for this connection has been growing over the past four decades, less than half of Americans recognize it as a risk factor for cancer, according to Surgeon General Dr. Vivek Murthy. “Alcohol is a well-established, preventable cause of cancer responsible for about 100,000 cases of cancer and 20,000 cancer deaths annually in the United States – greater than the 13,500 alcohol-associated traffic crash fatalities per year in the U.S. – yet the majority of Americans are unaware of this risk,” said Dr. Murthy said upon releasing the advisory on Jan. 3.
The advisory outlines the scientific evidence for the causal link between alcohol consumption and increased risk for such cancers as breast (in women; 16.4% of total breast cancer cases are attributable to alcohol consumption), colorectum, esophagus, voice box, liver, mouth, and throat. The type of alcohol being consumed – beer, wine, or spirits – does not matter, the admonition states.
Medical oncologist and hematologist Dr. Yael Zack, who founded and leads the Young Women’s Program for Cancer Care at White Plains Hospital’s Center for Cancer Care, has long advised against alcohol consumption and applauds the Surgeon General’s latest move. “For cancer prevention, we should avoid alcohol altogether,” she says, “but my general guidelines are to limit alcohol intake to 1-2 times per week, or even less frequently.”
Just as there is no “safe” number of cigarettes you can smoke per day, any amount of alcohol consumption can also raise your cancer risk.
Alcohol can damage your DNA in multiple ways as your body works to break it down, possibly resulting in mutations and DNA strand breaks which ultimately increase the risk of cancer, especially in tissues exposed to high levels of alcohol like the mouth and throat.
The timing of the Surgeon General’s advisory is made even more relevant by the annual arrival of “Dry January,” an initiative first developed by UK charity Alcohol Change UK in 2013. As its name suggests, the program challenges participants to forego all alcohol for the month of January, in the hopes that the resulting weight loss and other benefits may encourage curtailing or even eliminating alcohol use after Jan. 31.
Dr. Zack says that, in addition to Dry January, she recommends the following tips she learned from White Plains Hospital Registered Dietician Cheryl Leslie:
• Have alcohol-free days
• Find other outlets for relaxation instead of having an alcoholic beverage
• Don’t make having a glass of wine part of your food prep
• Limit alcohol consumption to only when socializing
• Alternate every other drink with a glass of water or seltzer
• Have a wine spritzer instead of a glass of wine
• Offer to be the designated driver at gatherings
• Enjoy many of the alcohol-free options that are now available These recommendations underscore how, for many people, one’s alcohol consumption can be prudently self-regulated. “Essentially I tell patients that since we have control over this risk factor, we should definitely take control,” Dr. Zack says.
These recommendations underscore how, for many people, one’s alcohol consumption can be prudently self-regulated. “Essentially I tell patients that since we have control over this risk factor, we should definitely take control,” Dr. Zack says.
Of course, self-management may not be sufficient in some cases. For those patients, Dr. Zack recommends consulting a therapist; a list of White Plains facilities can be found here.
Dr. Yael Zack is a medical oncologist and hematologist at the White Plains Hospital Center for Cancer Care and founded and leads the Young Women's Program for Cancer Care. To make an appointment with Dr. Zack, call 914.849.7600.
Health Matters
The original version of this article was published in Health Matters, a White Plains Hospital publication.
You Only Have One Heart: A Young Woman’s Journey to Better Health
- Details
- Written by: Joanne Wallenstein
- Category: Health
 Written by Dr. Anthony Mercando, Cardiologist at White Plains Hospital
Written by Dr. Anthony Mercando, Cardiologist at White Plains Hospital
Many of us know that having high cholesterol can increase one’s risk for heart disease and stroke, as it can build up plaque in the arteries. While high cholesterol can often be remedied with lifestyle changes, including alterations to diet and exercise, in many cases, a patient’s genetics play a role in their cholesterol levels, and medical intervention is needed.
Such was the case for Amanda Bulfamante, 33, a New Rochelle-based hairstylist who has a family history of cardiac events as well as high cholesterol. “I've never been able to get my cholesterol under control, even after changing my diet and losing weight,” she shares. When Amanda experienced heart palpitations, she made an appointment to see Dr. Anthony Mercando, a board-certified cardiologist at White Plains Hospital Physician Associates in White Plains.
“When Amanda came in, we reviewed her personal health history as well as her family history,” he says. “Since members of her family have experienced heart attacks at a young age, it was especially important to fully evaluate her risk.” To get the most accurate picture of Amanda’s heart health, Dr. Mercando ordered a long-term electrocardiogram test and blood test to check her cholesterol levels. In addition, he ordered a test known as a lipoprotein (a), or LP(a) test.
While Amanda’s heart palpitations proved to be benign and did not require treatment, two indications of elevated cardiovascular risk were evident from her blood tests. She had “a very high cholesterol level, and elevated levels of LP(a),” shares Dr. Mercando.
While there is currently no approved treatment for lowering LP(a), “an elevated value of LP(a) in a patient tells me that other risk factors and other lipids need to be aggressively treated,” he explains. High levels of LP(a) typically run in families as well are associated with arterial sclerosis, or hardening of the arteries.
As part of Amanda’s treatment plan, she now takes a statin medication to bring her cholesterol down in addition to continuing to eat a balanced diet and exercising regularly. “For many patients with a genetic predisposition to high cholesterol, even if they live the healthiest lifestyle possible, medication is needed to get their cholesterol to a healthy range and lower their risk for heart disease,” says Dr. Mercando.
Amanda was hesitant to start a medication regimen, especially given her young age. “I was concerned about potential side effects, but Dr. Mercando helped to put me at ease,” she shares. “I know that I am being as proactive as I can to stay healthy.”
Complicating matters even further was a near-simultaneous diagnosis of Multiple Sclerosis. “The DMT (disease-modifying therapies) I’m taking for the MS are very strong medications, and we continue to monitor how I react to that and the statin medications that Dr. Mercando put me on.”
Even with regular trips to a cardiologist and a neurologist, Amanda says she feels much better by getting checked early. “My advice would be to just go and get checked,” she declares. “It's really important. Some people may not take their heart health seriously because they think, ‘Oh, nothing's going to happen to me because I’m young and I don’t smoke.’”
“Taking care of yourself is so important,” she concludes. “You only have one heart.”
“I encourage everyone to discuss their family history of heart disease with their loved ones,” adds Dr. Mercando.  Dr. Anthony Mercando“Genetics play an important role heart health, and taking a proactive approach as Amanda has can make a meaningful difference in living a longer and healthier life.”
Dr. Anthony Mercando“Genetics play an important role heart health, and taking a proactive approach as Amanda has can make a meaningful difference in living a longer and healthier life.”
Click here to learn more about White Plains Hospital’s Cardiac Services Program.
Dr. Anthony Mercando is a board-certified cardiologist at White Plains Hospital Physician Associates. To make an appointment, call 914-849-4800.
Health Matters
The original version of this article was published in Health Matters, a White Plains Hospital publication.




















