How Men Can Reduce Their Cancer Risk
- Details
- Written by: Joanne Wallenstein
- Category: Health
 (Submitted by Kevin J. Wong, MD, Hematology & Oncology at White Plains Hospital)
(Submitted by Kevin J. Wong, MD, Hematology & Oncology at White Plains Hospital)
“Cancer” is a word that no one wants to hear from their doctor. While there is a regular stream of encouraging news when it comes to advancements in detection and treatment, the numbers of cancer occurrences continue to rise, and the American Cancer Society (ACS) projects that more than one million men will receive a cancer diagnosis in 2025.
Prostate cancer is the leading cancer type for men in the U.S., projected to represent 30% of diagnoses this year, followed by lung and bronchus cancer (12%), colorectal (7%), bladder (6%) and melanoma (6%).
It must be noted that, according to the ACS’ annual report on cancer facts and trends, overall cancer mortality has continued to decline, resulting in over 4 million fewer deaths in the United States since 1991. However, the organization warns, that progress is jeopardized by increasing incidence for 6 of the top 10 cancers as the projected number of new diagnoses in both men and women topped 2 million for the first time in 2024.
Lifestyle Changes and Early Detection: A Key to Better Outcomes
"We're encouraged by the steady drop in cancer mortality as a result of less smoking, earlier detection for some cancers, and improved treatment," said Rebecca Siegel, senior scientific director, surveillance research at the American Cancer Society and lead author of the report. "But as a nation, we've dropped the ball on cancer prevention as incidence continues to increase for many common cancers."
Early detection of any cancer can significantly improve chances of successful treatment and, therefore, survival; cancer care that is delayed or inaccessible lowers those chances and may ultimately result in higher costs of care. In addition, lifestyle changes can play a major role in reducing one’s cancer risk. Dr. Kevin Wong, a hematologist and oncologist at the White Plains Hospital Center for Cancer Care, recommends a number of important steps that men can take, including:
• Exercising regularly and maintain a healthy weight for your body type.
• Maintaining a healthy diet. “I recommend a diet high in fruits, vegetables, whole grains and low in saturated fats, red meat, processed foods and meats,” Dr. Wong says.
• Quitting smoking. “When going cold turkey doesn't work, discuss with your doctor tobacco-quitting aids and medications that can decrease cravings,” he says.
• Getting regular health screenings. “Follow up with your primary care doctor to make sure you are up to date with colonoscopy and other healthcare screenings at least once a year,” Dr. Wong recommends.
• Limiting alcohol. While the general recommendation is one drink per day for women, two drinks per day for men, “Zero is best,” he says.
• Getting regular exercise, “at least 3 times a week for 30 minutes where you are breathing a little hard during your routine,” Dr. Wong says, further recommending that anyone should always consult their physician before embarking upon a new exercise regimen. If you are experiencing any potential symptoms, see your physician as soon as possible. Remember that some cancers like prostate grow slowly and do not immediately present symptoms; Dr. Wong stresses that our primary care physician can be a great resource when determining which screenings are right for you. Remaining vigilant and being proactive are critical when it comes to the ongoing fight against cancer, regardless of age, gender or ethnicity.
If you are experiencing any potential symptoms, see your physician as soon as possible. Remember that some cancers like prostate grow slowly and do not immediately present symptoms; Dr. Wong stresses that our primary care physician can be a great resource when determining which screenings are right for you. Remaining vigilant and being proactive are critical when it comes to the ongoing fight against cancer, regardless of age, gender or ethnicity.
Learn more about White Plains Hospital's Center for Cancer Care.
Dr. Kevin Wong is a hematologist and oncologist at the White Plains Hospital Center for Cancer Care in White Plains. To make an appointment, call 914-849-7630.
Health Matters
The original version of this article was published in Health Matters, a White Plains Hospital publication.
When Should You Go to an Emergency Department?
- Details
- Written by: Joanne Wallenstein
- Category: Health
 (Submitted by Dr. Dean Straff, Director of Emergency Medicine)
(Submitted by Dr. Dean Straff, Director of Emergency Medicine)
Most people know that a severe medical situation requires a trip to their nearest hospital’s emergency department (ED). In some cases, however, people show up in the ED for reasons that are less urgent.
As the director of the busiest ED in Westchester County, I can confirm that most of our patients have chosen the right place. While less emergent issues such as a rash, a minor allergic reaction, or a sinus infection can be treated by your primary care physician or at a local urgent care facility, if the problem arises after hours, the safest option may be a visit to the ED.
Curious about what situations clearly call for a trip to the ED? Here are the top five:
1. Chest pain: If the pain lasts for more than five minutes, and/or is accompanied by shortness of breath, nausea, discomfort radiating to the arms, back, neck or jaw, it may signal a heart attack or other major cardiac event. Patients arriving with chest pain are promptly evaluated for a heart attack, acute heart failure, arrhythmia, and other related conditions. If we are able to rule out those events, we then consider less serious diagnoses like muscle strain or acid reflux.
2. Shortness of breath/difficulty breathing: Trouble breathing can be a a sign of a number of heart/vascular or lung/respiratory conditions such as heart attack, congestive heart failure, coronary artery disease, pneumonia, asthma, chronic obstructive pulmonary disease (COPD), or other infections.
3. High fever: Adults with a temperature of 102°F (38.9°C) or higher, especially with symptoms such as confusion, difficulty breathing, or severe pain; children with a temperature of 100.4°F (38°C) or higher, plus lethargy, difficulty breathing, loss of appetite, or a new rash; and infants under three months with any fever over 100.4°F (38°C) should contact their PCP immediately, or visit the ED if it is after office hours.
4. Stomach and abdominal pain, cramps and spasms: Sudden, severe, or persistent abdominal pain should never be ignored. Such symptoms could indicate appendicitis, gall bladder disease, bowel obstruction, kidney stones, or a foodborne illness – all requiring immediate evaluation.
5. Neurologic conditions: The sudden onset of severe neurological symptoms like headache, loss of consciousness, difficulty speaking, vision changes, weakness, and/or numbness can be signs of a stroke, brain aneurysm or other life-threatening condition, where timely treatment is essential.
Know Your Options
Please note that there are also urgent care facilities that may be right for some non-emergency situations, including the Urgent Care Center at White Plains Hospital Medical & Wellness in Armonk. I discuss some of the differences between what an ED does and what an urgent care center provides in this video. If you are uncertain whether your symptoms require emergency attention, always choose the Emergency Department. When in doubt, it is far better to be safe than sorry.
If you are uncertain whether your symptoms require emergency attention, always choose the Emergency Department. When in doubt, it is far better to be safe than sorry.
Dr. Dean Straff is the Director of Emergency Medicine at White Plains Hospital. If you are unsure about whether symptoms you or someone near to you are experiencing requires emergency attention, call 911.
Health Matters
The original version of this article was published in Health Matters, a White Plains Hospital publication.
Should You Invest in a Weighted Vest?
- Details
- Written by: Joanne Wallenstein
- Category: Health
 (Submitted by Dr. Mark Klion, Orthopedic Surgery at White Plains Hospital)
(Submitted by Dr. Mark Klion, Orthopedic Surgery at White Plains Hospital)
The latest workout trend is wearing a weighted vest. Once a tool for soldiers and policemen, weighted vests today seem to be everywhere – you may see them in use at the gym, on a leisurely walk, or even at your workplace. It seems that everybody from your friend to your postman and even your physician (yes, that includes me) is trying one on for size.
But is the weighted vest something destined to go the way of high-fat diets, the ThighMaster, and the Jazzercise class – or is it something with a high longevity potential? In this article, I will review its history, how it works, and the pros and cons of wearing one.
Ten-Hut!
The weighted vest actually dates back to such civilizations as the ancient Greeks, who filled leather vests with sand or stones to help train their soldiers for combat. Likewise, vests are used by many of today’s military and police units to simulate the extra weight of body armor and equipment during training exercises.
The term “rucking” also originates with the military, and refers to a walking with weight on your back – typically in a backpack, a.k.a. a rucksack. The term is now common among the vest-wearing public.
How Does It Work?
Walking with a weighted vest is a low impact exercise that spreads the weight evenly across the body, rather than simply holding free weights. It is recommended that, when starting off, you use weights between 5% and 10% of your body weight for the best effect; otherwise, you risk straining your muscles and/or joints. Once your body has gotten used to this regimen, you may increase the weight by 2% to 5% of your body weight. However, a maximum of 15% is the general rule of thumb, though you may be able to surpass that with experience and a consultation with your physician.
How often should you wear the vest? I recommend two to three times a week, for up to 60 minutes during an exercise session or a maximum of three hours if you are walking. Wearing it all day is very inadvisable, as the extra weight on your back and joints will ultimately pose problems.
Pros
The idea behind wearing a weighted vest is to improve strength, stamina, and overall fitness, as well as potentially lose weight through additional burning of calories. The weighted vest can also benefit those who suffer from osteoporosis. Using the vest can help to build bone density and muscle strength, thus reducing the risk of a fracture, and can positively affect your balance.
As with any new exercise regimen, moderation is key; only by gradually increasing the weight in the vest, and by carefully increasing the length of your workout (walking, calisthenics, etc.), will you realize the greatest benefit. If at any point you feel pain or other uncomfortable side effects, reduce the weights to your former level; if the pain continues, you should see a physician to determine if you may have injured yourself.
Cons
If you suffer from arthritis, particularly in the back and/or knees, proceed carefully. While a weighted vest can help with bone density, muscle strength, and endurance, its use may also aggravate joint pain and strain in the knees, hips and lower back. You may also experience a negative impact on your posture, in which case you probably are carrying too heavy a burden. Either way, discuss with your physician whether a weighted vest – or perhaps some other equipment – may be the best way for you to achieve your exercise goals. A medical professional is always your best resource when it comes to exploring new options.
Either way, discuss with your physician whether a weighted vest – or perhaps some other equipment – may be the best way for you to achieve your exercise goals. A medical professional is always your best resource when it comes to exploring new options.
Dr. Mark Klion is a board-certified Orthopedic Surgeon specializing in Sports Medicine at White Plains Hospital Physician Associates (WPHPA) Orthopedic Surgery in West Harrison. To make an appointment, call 914-849-7897.
Health Matters
The original version of this article was published in Health Matters, a White Plains Hospital publication.
Life-Saving Pregnancy Care at White Plains Hospital
- Details
- Written by: Joanne Wallenstein
- Category: Health
 When Alissa Cheperak’s pregnancy took a turn, the expert care at White Plains Hospital made a life-saving difference for both her and her daughter.
When Alissa Cheperak’s pregnancy took a turn, the expert care at White Plains Hospital made a life-saving difference for both her and her daughter.
When Cheperak discovered she was pregnant, she and her husband, Scott, were ecstatic. The Ossining-based couple were thrilled that their hoped-for timing had worked out, and they knew exactly where to get the best obstetrical care in the region.
As a social worker and a certified case manager at White Plains Hospital, Alissa was already familiar with the world class expertise at the Hospital. She soon found the perfect doctor to see her through the next nine months: OB/GYN Dr. Dana Bryant.
Subtle Symptoms of Major Trouble
Cheperak sailed through her pregnancy, but in July, she began to feel unwell. “One Tuesday night, I woke up with what felt like heartburn” she recalls, “I thought, ‘I’m pregnant, and its common.’”
The next day, the pain persisted. Dr. Bryant suggested an over-the-counter antacid, then a slightly stronger version when the first didn't help. Still, Cheperak’s symptoms worsened.
A Worsening Situation
That Friday, Dr. Bryant got another call from Cheperak. “She described pain wrapping around her rib cage and radiating to her back,” Dr. Bryant says. “I advised her to go to the Emergency Department.” At White Plains Hospital, a chest X-ray and CAT scan ruled out a heart attack and pulmonary embolism, but blood tests revealed something more serious — Cheperak had HELLP syndrome:
• HELLP syndrome (hemolysis, elevated liver enzymes, and low platelet count) is a rare and potentially life-threatening pregnancy complication.
• Affecting fewer than 1% of pregnant women, HELLP can cause dangerously high blood pressure, organ dysfunction, and severe complications; as many as 24% of affected mothers and 34% of babies do not survive.
While Cheperak was seriously ill, she had not yet reached a critical stage. There is only one cure for HELLP; delivery of the baby. In Cheperak’s case, it meant giving birth very early-at 27 weeks.
Dr Bryant didn't rush Cheperak into the operating room. As soon as she was stable, Dr. Bryant performed a C-section. Cheperak’s baby, Claire, entered the world at a mere 1 lb. 10 oz.
“They showed her to us very quickly, because they had to get her hooked up to oxygen,” Cheperak says, overcome with emotion.
Unbeatable Care
Claire spent two long months in White Plains Hospital’s neonatal intensive care unit (NICU). Whether Cheperak’s daughter needed a blood transfusion, or to have her oxygen level increased, someone was on hand to carefully make sure the task was performed.
Like many preemies, Claires health was unstable at first. When, after a month, Claire showed signs of abnormal development of blood vessels of the retina, her care team at White Plains Hospital recommended she be transferred to a hospital where she could receive even more specialized care.
Because White Plains Hospital is a part of the Montefiore Health System, Claire was able to be transferred to Montefiore Medical Center’s Wakefield Campus, where her care would continue within the same network, providing a consistent approach to treatment during a critical time.
A Triumphant Homecoming
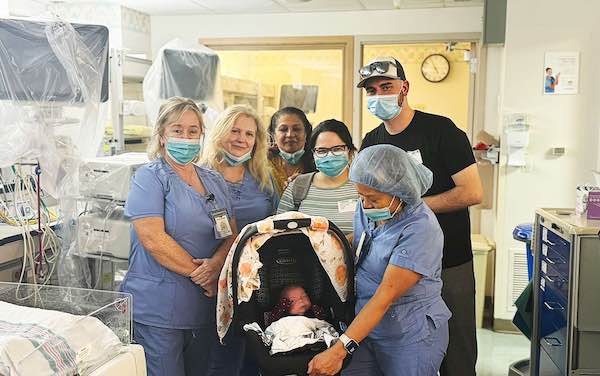
Three months after her birth, Claire was finally ready to go home. Although she requires physical therapy, the nearly 11-month-old has been thriving from the day she arrived home.
Dr. Bryant praises Cheperak for keeping in touch as her condition worsened during the pregnancy. “If your doctor is treating you for a more common symptom, such as heartburn, and it still isn’t getting better, always be willing to speak up,” Dr. Bryant says.
Still, she adds, pregnant women shouldn’t panic if they suffer from heartburn-like sensations. “Most women aren’t going to develop HELLP syndrome,” she stresses. But there’s no better place to seek assistance than at the Hospital, she says: “We have the specialized expertise to quickly assess your situation and help you fully understand whether it is something to be concerned about, or just a normal symptom in a long pregnancy.”
Cheperak and her husband experienced firsthand how even the most carefully planned pregnancies can take unexpected turns. They feel eternally grateful for the care they received at White Plains Hospital when both mother and baby’s lives were on the line.
Learn more about Maternity Services at White Plains Hospital.
Health Matters
The original version of this article was published in Health Matters, a White Plains Hospital publication.
Behind the Trend: Fitness Trackers
- Details
- Written by: Joanne Wallenstein
- Category: Health
 Submitted by Daniel Silovitz, DO, Internal Medicine
Submitted by Daniel Silovitz, DO, Internal Medicine
Fitness bands, smart watches, and even smart rings have flooded the market in recent years.
These popular devices use sensors to help wearers track a variety of health metrics and can be an effective tool to kickstart or monitor your fitness routine, says Dr. Daniel Silovitz, an Internal Medicine Physician with White Plains Hospital Physician Associates.
While step counters are one of the most popular features, modern trackers can monitor more, so wearers should decide what they want to keep track of when shopping for a device.
Some models can be used to keep an eye on important variables in your overall health including:
• Heart rate
• Sleep duration and quality
• Cardiorespiratory fitness levels (helpful for serious workout enthusiasts looking to increase their VO2 max, or maximum oxygen consumption, which it estimates based on your heart rate and distance traveled).
“These devices can be a great way to keep track of your overall health and performance, but they do have limitations,” warns Dr. Silovitz. “They shouldn’t replace going to see your physician.”
Many devices can detect an irregular heartbeat, which may indicate Atrial Fibrillation (AFib), which may have no symptoms and can increase one's risk of stroke and heart failure. Dr. Silovitz also points out that the more you wear these devices, the better they’ll become at synthesizing your personal health data, so consistency is key. Learn more about White Plains Hospital Physician Associates' Internal Medicine and Primary Care Services.
Learn more about White Plains Hospital Physician Associates' Internal Medicine and Primary Care Services.
Dr. Daniel Silovitz is an internal medicine physician at WPHPA of Harrison, specializing in preventive medicine and the management of chronic conditions. To make an appointment, call 914.835.0073.
Health Matters
The original version of this article was published in Health Matters, a White Plains Hospital publication.











